Staffing Stability: Why It Matters for Surgical Procedures
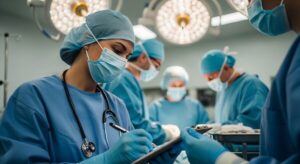
Surgical care depends on more than clinical expertise alone. Behind every procedure is a coordinated team working together in a highly structured environment. Staffing stability refers to more than maintaining coverage. It reflects how consistently teams work together over time, how well they understand the dynamics of a specific facility and how effectively they coordinate within the operating room. When stability is disrupted, the effects can extend into multiple areas of care, influencing efficiency, communication and patient outcomes.
What staffing stability means in a surgical setting
In surgical environments, staffing stability involves maintaining a consistent team of clinicians who are familiar with the workflows, expectations and culture of a facility. It includes low turnover, limited reliance on temporary coverage and long-term alignment between providers and the organization.
Stable teams develop a shared understanding of how care is delivered within a specific setting. They become familiar with surgeon preferences and procedural patterns. This consistency allows teams to operate with greater efficiency and fewer disruptions. When staffing is less stable, teams may need to continually adjust to new individuals, communication styles and approaches to care. Even when clinicians are highly experienced, the absence of familiarity can introduce variability into the workflow.
Impact on operating room efficiency
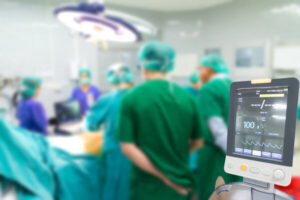
Operating room efficiency is closely tied to how well surgical teams work together. Established teams often develop predictable routines that support consistent case flow throughout the day. First case starts are more likely to remain on schedule, and turnover times between procedures tend to be more consistent. When team members understand one another, many aspects of the workflow require less active coordination. Anticipation replaces repetition, and small logistical details are handled more seamlessly. Over the course of a full surgical schedule, these incremental efficiencies can have a measurable impact.
In contrast, frequent staffing changes can slow down this process. Teams may need additional time to confirm preferences, clarify communication or adjust to different working styles. While these adjustments are manageable, they can accumulate and affect overall throughput.
Team communication and coordination
Clear communication is important in any surgical setting. Stable teams develop efficient communication patterns that support routine procedures and emergency situations. Team members learn how colleagues prefer to exchange information, when to anticipate key steps and how to respond quickly and appropriately when conditions change.
When staffing is inconsistent, communication becomes less predictable. New team members may not be familiar with established processes. This can lead to more frequent clarifications, repeated instructions or minor delays as teams work to stay aligned. Over time, strong communication within stable teams contributes to smoother coordination and a more predictable and efficient surgical environment.
Consistency and patient safety
Patient safety and consistency in care delivery are closely connected. Stable surgical teams are more familiar with facility-specific protocols, equipment and emergency procedures. This familiarity allows them to respond efficiently and keep a high level of situational awareness throughout each case. Continuity also reduces the number of handoffs within the care process. Fewer transitions can reduce the risk of miscommunication and support consistent patient monitoring from start to finish. While experienced clinicians can deliver safe care in a variety of settings, consistency within a dedicated team reduces variability and reinforces established safety practices.
The limitations of temporary staffing models
Temporary staffing solutions can help maintain coverage during periods of transition or workforce shortages. However, these models introduce variability into the surgical environment. Rotating clinicians may not have the same level of familiarity with a facility’s workflows, team dynamics or operational expectations. This can result in teams spending additional time aligning on processes that would otherwise be routine.
Temporary coverage can address immediate staffing needs, but it does not always provide the continuity required for long-term operational consistency. Facilities that rely heavily on short-term staffing may find it more challenging to maintain the same level of efficiency and coordination over time.
How staffing stability supports surgical program growth
Stable staffing provides a foundation for growth within surgical programs. When teams are consistent and coordinated, facilities are better positioned to expand services, increase case volume and support new procedural areas.
Surgeons and administrative leaders often rely on predictable support from surgical teams. Confidence in staffing consistency allows organizations to scale operations while maintaining performance. A consistent environment supports stronger professional relationships and a more structured workflow, which can influence long-term engagement.
Why staffing stability matters
Staffing stability is an important part of surgical performance. It influences how efficiently operating rooms function, how effectively teams communicate and how consistent care is delivered to patients.
Collaborative Anesthesia Partners works with hospitals, ambulatory surgery centers and office-based practices to build stable, well-coordinated surgical teams that support efficient operations and high-quality patient care. See how a more stable surgical team can strengthen overall performance.